To understand why you need endodontic treatment, it helps to know something about the anatomy of the tooth. Teeth are composed of three layers, the outer enamel, the inner dentin and the innermost layer, the pulp. The enamel is the outer insulating layer of the tooth that is devoid of nerve supply. The next layer, the dentin is innervated and is the sensitve tooth structure. The pulp contains blood vessels, nerves, and connective tissue and creates the surrounding hard tissues of the tooth during development. The pulp is housed in the canal system within the tooth, which comprises of the pulp chamber in the crown and the root canals in the roots. The pulp connects to the tissues surrounding the root through the apex or the tip of the roots.
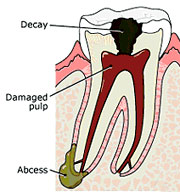
Endodontic treatment is necessary when the pulp becomes inflamed or infected. The inflammation or infection can be due to a variety of causes: deep decay, repeated dental procedures on the tooth, or a crack or chip in the tooth or traumatic injury to the tooth. If pulp inflammation or infection is left untreated, it can cause pain or lead to an abcess.
Signs of pulp damage include throbbing pain, prolonged sensitivity to heat or cold, discoloration of the tooth, swelling and tenderness in the nearby gums. Sometimes, there are no symptoms.
Endodontic treatment can often be performed in one or two visits depending on the complexity of the canal system and the severity of the infection. It involves the following steps:
1) The endodontist examines and performs several tests to determine the pulpal status, x-ray the tooth, then administers local anesthesia. After the tooth is numb, the endodontist places a small protective sheet called a "dental dam" over the area to isolate the tooth and keep it clean and free of saliva during the procedure.
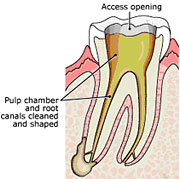
2) The endodontist makes an opening in the crown of the tooth to acess the pulp chamber and locates the root canals. Anterior teeth and lower bicuspids usually have one canal, upper bicuspids usually have two canals and the molars have 3-5 canals. Very small instruments called files are used seqentially to clean and shape the canal system to receive the canal filling.
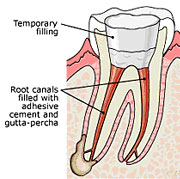
3) After the space is cleaned and shaped, the endodontist fills the root canals with a biocompatible material, usually a rubber-like material called "gutta-percha." The gutta-percha is placed with an adhesive cement to ensure complete sealing of the root canals. In most cases, a temporary filling is placed to close the opening. The temporary filling will be removed by your dentist before the tooth is restored.
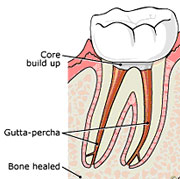
4) After the final visit with your endodontist, you must return to your dentist to have a crown or other restoration placed on the tooth to protect and restore it to full function. Failure to do so will result in fracture of the tooth and ultimate loss of the tooth.
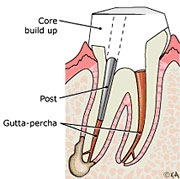
5) If the tooth lacks sufficient structure to hold the restoration in place, your dentist or endodontist may place a post inside the tooth. Ask your endodontist for more details about the specific restoration planned for your tooth.